Table of contents
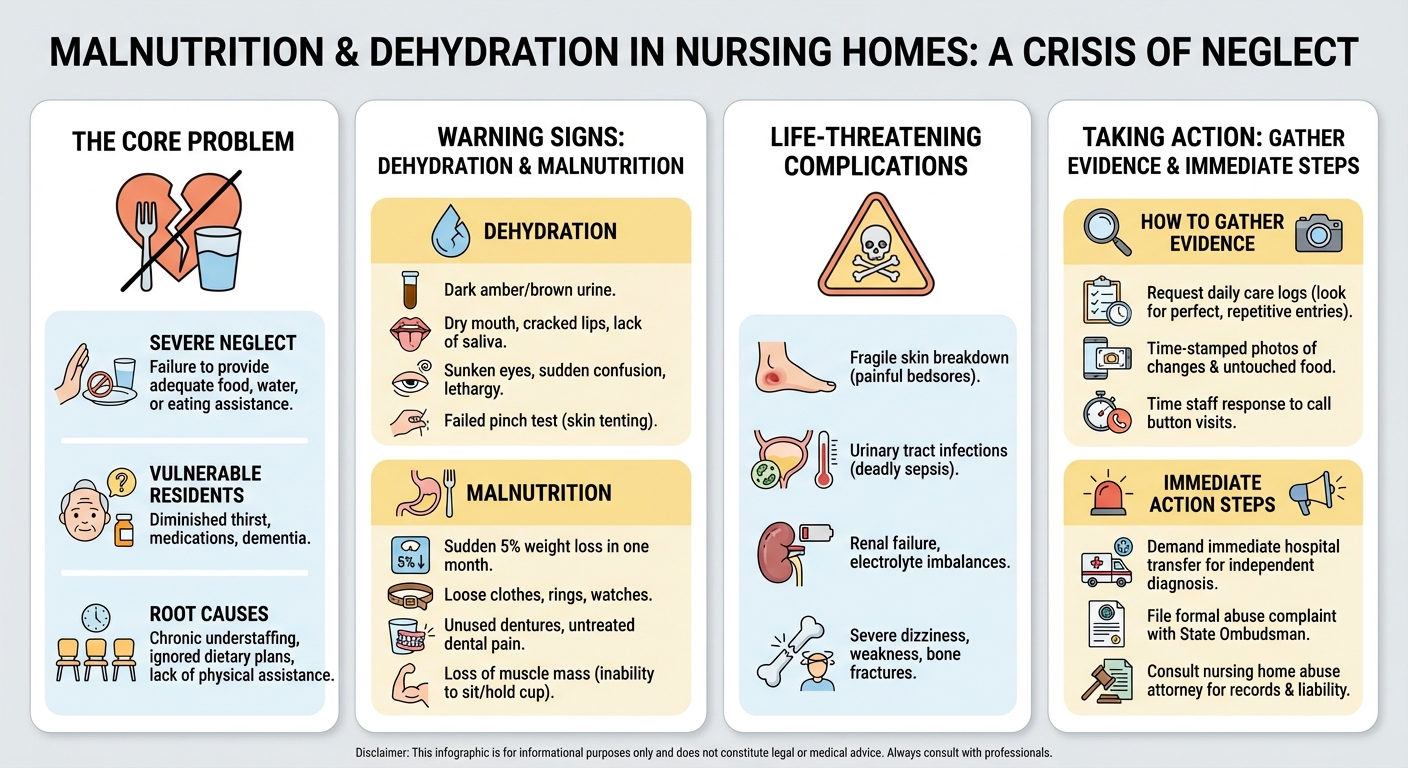
Malnutrition and dehydration in nursing homes are severe forms of neglect that occur when staff fail to provide adequate food, water, or eating assistance. Warning signs include sudden weight loss, dark urine, dry mouth, confusion, and poor skin elasticity. If left untreated, these conditions can cause life-threatening complications like kidney failure, sepsis, and bedsores.
The Hidden Crisis: Malnutrition and Dehydration in Nursing Homes
Placing a loved one in a nursing home comes with the expectation that their most basic human needs—food and water—will be met. Unfortunately, nursing home malnutrition and dehydration remain a hidden crisis in facilities across the United States. When staff fail to provide adequate nourishment and hydration, vulnerable residents can suffer rapid, life-threatening physical and cognitive declines.
Why the Elderly Are Highly Vulnerable
Older adults naturally face a higher risk of malnutrition and dehydration. As people age, their natural thirst mechanism diminishes, meaning they may not feel thirsty even when their bodies desperately need fluids. Additionally, many elderly residents take medications like diuretics that increase fluid loss, or suffer from dementia, which can cause them to forget to eat or drink.
The Difference Between Natural Decline and Facility Neglect
While aging brings inevitable health challenges, sudden or severe weight loss and dehydration are rarely just “part of getting older.” Natural decline happens gradually and is carefully monitored and managed by medical professionals. Facility neglect occurs when a nursing home fails to implement a care plan, ignores a resident’s inability to feed themselves, or lacks the staff to ensure residents are actually consuming their meals and fluids.
Critical Warning Signs of Dehydration in Elderly Residents
Dehydration can escalate from mild to severe in a matter of hours. Families must be vigilant during visits and watch for the following warning signs.
Physical Symptoms (Skin Turgor, Dry Mouth, Dark Urine)
- Dark Urine: Urine should be pale yellow. Dark amber or brown urine is a late-stage warning sign of severe dehydration.
- Dry Mouth and Cracked Lips: A lack of saliva, difficulty speaking, or severely chapped lips indicate a lack of fluids.
- Sunken Eyes: The skin around the eyes may appear hollow or unusually dark.
Cognitive and Behavioral Changes (Sudden Confusion, Lethargy)
If your loved one is suddenly confused, disoriented, or unusually exhausted, do not automatically attribute it to dementia or aging. Dehydration causes a rapid drop in blood volume, reducing oxygen to the brain and leading to sudden delirium, lethargy, or unresponsiveness.
The ‘Pinch Test’ and Other Quick Checks
You can perform a quick check for dehydration using the “pinch test” (checking skin turgor). Gently pinch the skin on the back of your loved one’s hand or lower arm. In a well-hydrated person, the skin snaps back immediately. If the skin remains “tented” or takes several seconds to flatten out, the resident is likely dehydrated.
Red Flags for Malnutrition in Nursing Care
Malnutrition occurs when a resident does not get enough calories, protein, or essential nutrients. It is a slow, dangerous process that weakens the immune system and destroys muscle mass.
Unexplained Weight Loss and Loose Clothing
The most obvious sign of malnutrition is a sudden drop in weight. If you notice your loved one’s clothes, rings, or watches fitting much looser than usual, or if their face appears gaunt, demand to see their recent weight logs. A loss of 5% of body weight in a month or 10% in six months is a major clinical red flag.
Dental Issues and Unused Dentures
Many elderly residents require dentures or have poor dental health, making chewing painful. If a nursing home fails to provide a soft-food diet as prescribed, the resident may simply stop eating. Check if your loved one’s dentures are clean, properly fitted, and actually being worn during meal times.
Weakness, Fatigue, and Loss of Muscle Mass
A lack of protein leads to muscle wasting (sarcopenia). If a resident who could previously stand or walk with assistance suddenly lacks the strength to sit up in bed or hold a cup, severe malnutrition may be the underlying cause.
Severe Complications: When Poor Care Becomes Life-Threatening
When nursing homes fail to provide food and water, the cascading health effects can be fatal.
Bedsores (Pressure Ulcers) and Slow Wound Healing
Skin requires water and protein to maintain its integrity. Malnourished and dehydrated residents have fragile skin that breaks down quickly under pressure, leading to painful bedsores. Without proper nutrients, these ulcers cannot heal and often progress to the bone.
Urinary Tract Infections (UTIs) and Sepsis
Without enough water to flush out bacteria, residents are highly susceptible to Urinary Tract Infections (UTIs). In the elderly, an untreated UTI can quickly travel to the kidneys and bloodstream, resulting in sepsis—a life-threatening systemic infection.
Kidney Failure and Electrolyte Imbalances
Severe dehydration forces the kidneys to work overtime. This can lead to acute kidney injury or complete renal failure. It also causes dangerous electrolyte imbalances (like high sodium or potassium levels), which can trigger fatal heart arrhythmias.
Increased Fall Risk and Bone Fractures
Weakness from malnutrition and dizziness from dehydration are a disastrous combination. Residents in this state are at a significantly higher risk of falling, which frequently results in devastating hip fractures or traumatic brain injuries.
Root Causes: Why Do Facilities Fail to Hydrate and Feed Residents?
Understanding why this neglect happens is crucial for holding the right parties accountable.
Chronic Understaffing and High Turnover
The number one cause of nursing home neglect is understaffing. Corporate cost-cutting often leaves too few aides to care for too many residents. Feeding a resident with cognitive or physical impairments can take 30 to 45 minutes. Overworked staff may simply leave food trays out of reach or take them away before the resident has finished eating.
Failure to Follow Individualized Dietary Care Plans
Every resident must have a federally mandated care plan that outlines their dietary needs. If a resident requires thickened liquids to prevent choking, or a pureed diet, staff must provide it. Neglect occurs when temporary or untrained staff ignore these specific, life-saving instructions.
Lack of Assistance for Residents with Mobility or Swallowing Issues
Conditions like Parkinson’s, stroke, or advanced Alzheimer’s can cause dysphagia (difficulty swallowing) or a loss of motor skills. These residents cannot physically feed themselves or open water pitchers. If staff do not actively assist them, they will starve and dehydrate, even if a full tray of food is placed directly in front of them.
How to Gather Evidence of Malnutrition or Dehydration
If you suspect neglect, you must act quickly to document the situation before evidence disappears.
Requesting and Reviewing Daily Care and Hydration Logs
Nursing homes are required to document food and fluid intake. Request copies of these logs. Look for generic, repetitive entries (e.g., “ate 100% of meal” every single day) which often indicate staff are filling out charts without actually monitoring the resident.
Documenting Physical Changes (Photos and Weight Charts)
Take time-stamped photos of your loved one’s physical condition, including dry lips, sunken eyes, or loose skin. Photograph untouched food trays left out of reach. Request the facility’s official weight charts to prove a timeline of sudden weight loss.
Tracking Staff Response Times During Visits
Use the call button during your visit and time how long it takes for staff to respond. If it takes 30 minutes for an aide to bring a requested glass of water while family is present, it is highly likely the resident is being ignored when family is absent.
Immediate Steps to Take if You Suspect Neglect
Do not wait for the facility to correct the issue on its own. Take these steps immediately to protect your loved one.
1. Demand Immediate Medical Intervention
If your loved one is showing signs of severe dehydration or malnutrition, demand that they be transferred to a hospital immediately. An independent emergency room doctor can officially diagnose dehydration or malnutrition, providing critical medical documentation of the neglect.
2. Report the Facility to the State Ombudsman
File a formal complaint with your state’s Long-Term Care Ombudsman and the state department of health. This triggers an official investigation into the facility’s practices and creates a public record of the abuse.
3. Consult a Nursing Home Abuse Attorney
Once your loved one is medically safe, speak with a lawyer who specializes in elder abuse. They can help you subpoena internal facility records, hold the nursing home financially accountable, and seek compensation for medical bills and suffering. For more information on what to expect financially, read our guide on How Much Can You Sue a Nursing Home for Negligence?
Frequently Asked Questions About Nursing Home Neglect
Is dehydration always a sign of nursing home neglect?
Not always, but it is a strong indicator. While certain medications or illnesses can increase the risk of dehydration, a properly staffed nursing home should monitor fluid intake and intervene medically before dehydration becomes severe.
How long does it take for severe dehydration to cause permanent damage?
Severe dehydration can cause permanent organ damage, particularly to the kidneys and brain, in a matter of days. In frail, elderly residents, the window for intervention is incredibly short, making immediate medical care essential.
Can a nursing home be held liable for a resident’s weight loss?
Yes. If the weight loss is the result of the facility failing to follow the resident’s dietary care plan, failing to provide eating assistance, or ignoring signs of malnutrition, the nursing home can be held legally and financially liable for neglect.